St. Petersburg is one of the biggest research and education centers in Russia with over 10% of the country’s scientific potential situated here, represented by over 350 institutions. Three scientists working in the city were invited to take part in the 32nd installment of the Break Down by Atoms lecture series organized by the Informational Center for Atomic Energy: Natalia Katolikova, junior research associate at the Institute of Translational Biomedicine of St. Petersburg State University, Margarita Tyupina, a researcher at the Laboratory of Theoretical Chemistry of the Khlopin Radium Institute, and Mikhail Kurushkin, dean of ITMO’s Faculty of Biotechnologies.
Here is a recap of the presentations.
Radiation that saves lives
Margarita Tyupina, a researcher at the Laboratory of Theoretical Chemistry of the Khlopin Radium Institute, gave an overview of the history of using radiation to treat cancer and outlined the fields where nuclear medicine is developing these days.
It was actually Maria Skłodowska-Curie who first thought of radium’s healing properties. Back in 1922, she founded the first Institut du Radium in Paris – now known as Curie Institute. Then, in 1932, two years before her death, she founded the Institute of Radium in her home Warsaw. Later, it became the Institute of Oncology and now is also named after her.

The initial push for the development of this method was the discovery of the radioactive tracers method by Hungarian physicist George de Hevesy and Austrian-born chemist Friedrich Paneth in 1913. Using this method, scientists link a stable chemical element to a radioactive one, which is hard to measure and trace. Contemporary high-tech medicine is based on this method.
Essentially, isotopes are the same element but with a different molar mass (due to a different number of neutrons in their atoms). We now know almost 3,000 isotopes, only 10% of which are stable.
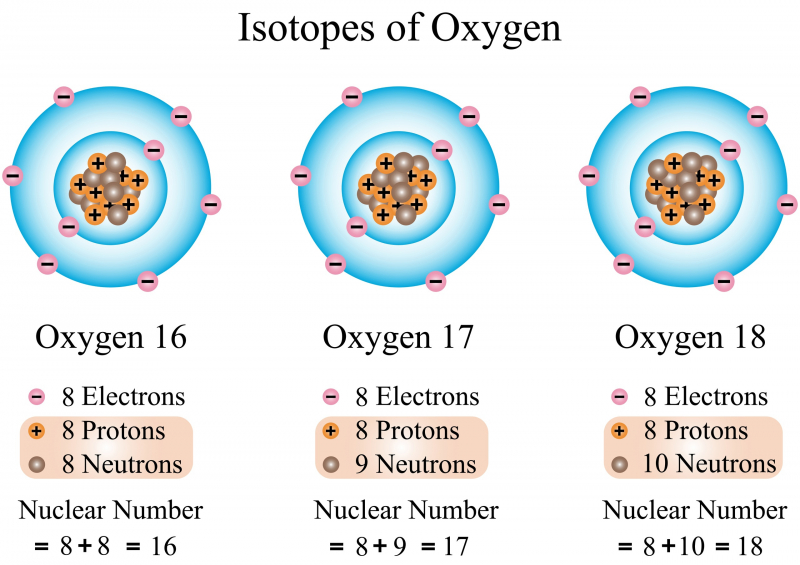
Isotopes can’t be put inside the human body – first, they need to be packed into a so-called pharmaceutical product. These products are made of two parts: the radionuclide and the guiding substance.
There are three main fields in nuclear medicine: diagnostics, treatment, and the newly added theranostics. Diagnostics mainly employs two methods: radioimmune analysis in vitro, when a blood sample is analyzed, and in vivo, when the treatment is injected into the body – positron emission tomography (PET) and single-photon emission computed tomography (SPECT). PET uses beta plus isotopes, which emit several gamma quanta with a short half-life period. SPECT is a more widespread technology that uses radiopharmaceutical agents that emit only one gamma quantum. One of the popular agents is technetium – it allows to run diagnostics for almost every organ.
There are two types of treatment: brachytherapy, when the treatment is injected directly into the affected organ, and radiation treatment, when the patient is put near the isotope which shines at the tumor.
Theranostics, the brand new trend of the early 21st century, brings together diagnostics and therapy and offers a more efficient personalized treatment. The only isotope now in its preclinical stage is iodine-131 that detects malignant cells in the vascular system and instantly kills them.
There are five main nuclear medicine research centers in Russia: the Kurchatov Institute and the Institute for Theoretical and Experimental Physics in Moscow, the Institute for High Energy Physics in Protvino, St. Petersburg Nuclear Physics Institute in Gatchina, and the Khlopin Radium Institute in St. Petersburg. At the same time, Russia is among the top five producers of raw medical isotopes in the world.

The Khlopin Radium Institute manufactures six pharmaceutical agents that cover 95% of the city’s demand. The institute is also conducting research: at the end of 2021, the clinical trials of an agent analogous to the German Xofigo (radium-223 dichloride) that is used to treat metastatic tumors of the skeleton. One dose of Xofigo costs around 1.5 million rubles – and three such doses are needed to get rid of the metastases in the skeleton. Researchers at the institute developed a new way to produce radium dichloride that will decrease the cost by five times. The first supplies of the treatment are expected in 2024. The Laboratory of Actinide Chemistry is also working to develop new options with technetium isotopes: technetium-99m petracarbanilide for perfusion diagnostics and lung ventilation and technetium-99m carbonyl with a fatty acid for diagnosing metabolic processes in the myocard.
ITMO’s first citizen science project
Mikhail Kurushkin, dean of ITMO’s Faculty of Biotechnologies talked about the Internet of Bacteria project launched by the university’s SCAMT international research center and Kuban State University (KubSU).

The Internet of Bacteria project focuses on studying microbial fuel cells which use dirt or soil as electrolytes. For the project to succeed, it requires collecting as much data as possible on bacterias that produce electric energy and the soils they populate. To test the hypothesis requires getting a large number of people involved, which can be done through citizen science.
Only a small fraction of existing microorganisms are studied by scientists around the world. The research group behind the project is interested in those bacteria that have high levels of electric activity – to describe these organisms, identify the mechanism of electriс activity, and later use this knowledge for genome research.

The project was launched in 2020 and entered its active stage in late November, when 100 fuel elements were sent to 17 bioquantoriums in Russian cities. These sets had four jars with different types of soil – for instance, with ferruginous soil to demonstrate what to look for and with regular peat soil for comparison. The sets also included a microprocessor board that can connect to a cloud server, as well as an analog-to-digital converter.
It’s important to mention that the key people behind the project are students: Andrey Lazukin, a Master’s student at KubSU is lead engineer, and Daria Minakova, a third-year Bachelor’s student at the Faculty of Biotechnologies, is the main coordinator of the project.
How stem cells help treat Parkinson’s disease
Natalia Katolikova, junior research associate at the Neurobiology and Molecular Pharmacology Laboratory at the Institute of Translational Biomedicine of St. Petersburg State University, talked about how researchers found a way to grow artificial stem cells and how this discovery can help treat neurodegenerative illnesses, such as Parkinson’s disease.

We live in the age of rapidly advancing medicine: we learn more and more about diseases and their development, as well as find new ways to treat them. We have learned to extend the human lifespan – but with this comes a new issue, that we are faced with new diseases, including neurodegenerative ones, common amongst the elderly. The most well-known of them are Parkinson’s disease and Alzheimer’s disease. Unfortunately, they are becoming more and more common even among such famous people as Muhammad Ali, Michael J. Fox, or Margaret Thatcher. We know next to nothing about the reasons behind the onset of these diseases, we have a poor understanding of why they happen, and can’t really treat them.
Parkinson’s disease involves the death of a specific type of neuron, dopaminergic ones, in one specific place – the substantia nigra located in the midbrain. This leads to a significant drop in the production of dopamine, which is an important mediator regulating many processes in our body, including motor functions. That is why the disease has such characteristic symptoms.
Right now the main treatment of Parkinson’s disease deals only with these symptoms. It usually involves drugs that contain dopamine predecessors or the mediator itself, which interacts with receptors and alleviates the symptoms for a short while. But such treatment doesn’t help to cure the disease and fight the very reason behind it, so the disease just keeps progressing. The whole cycle – from the start of therapy to complete disability takes about 5-6 years.

So, researchers came up with an idea – why don’t we replace the dead cells with healthy neurons? The first such experiment was conducted in Sweden in the 1970s – several patients received cells from embryos. This eliminates the symptoms and allows the patients to spend five years without taking medication. Researchers got the chance to examine these patients during their whole lives, which led them to notice that the new neurons also degraded with time. But given that this illness is more common in old age, five-six years of comfortable symptomless living without the need to take any medication is a significant win.
The main problem of this method is that it’s impossible to find the source of cells for such transplantation. Of course, we can take cells from a pig – they are similar to human ones, but they still function differently. We can take the cells from a healthy person – but who in their right mind will agree to this? And it is impossible to transplant cells of a human embryo – it is prohibited and considered unethical in the majority of countries.

The only remaining option is to use stem cells. They are remarkable in the fact that there is no limit to their division and they can be grown into any tissue or organ. However, the public opinion on such experiments has drastically changed since the discovery of stem cells in 1998. New laws are now in force in the USA that prohibit breeding new types of stem cells – this has hindered the work of scientists and brough many research fields to an end.
It all changed in 2006, when Shinya Yamanaka from Kyoto University discovered the way to artificially bring the already differentiated cell back to the state characteristic of stem cells. He called them induced pluripotent stem cells and already in 2012 received a Nobel Prize in Physiology and Medicine.
Initially, Yamanaka experimented with retina cells – they adapt the best when transplanted, so they are the easiest to use in clinical trials. It quickly became clear that the new technology has a great potential in treating neurodegenerative illnesses, in particular, Parkinson’s disease. There are currently several research groups doing research in this field – clinical trials started in Japan and the USA in 2018 and 2020 respectively and they are soon to start in the UK and Sweden.
This method is currently not studied in Russia. Researchers at the Neurobiology and Molecular Pharmacology Laboratory can work with induced pluripotent stem cells and acquire dopaminergic neurons that can be transplanted to animals. Similar projects are conducted in a huge spectrum of fields: the treatment of heart diseases, degenerative illnesses of joints and pancreas, as well as diabetes.
You can watch the whole event here (in Russian).